Asherman’s Syndrome Treatment
Home > Specialities > Asherman’s Syndrome Treatment
Asherman’s Syndrome is also known as “intrauterine adhesions” or “intrauterine synechiae." It happens when scar tissue (adhesions) grows inside your uterus (womb) and/or cervix. This scar tissue most often develops after procedures (such as dilation and curettage (D&C)) that remove tissue from your uterus.
The severity ranges from mild to severe based on adhesion extent, and it can be a serious condition. The symptoms may look like very light periods (hypomenorrhea), no period (amenorrhea), severe menstrual cramping (dysmenorrhea), pelvic pain, difficulty getting pregnant (uterine factor infertility), and recurrent miscarriages.
If you are experiencing these symptoms, especially after a dilation and curettage procedure, go for an expert evaluation at the Best Asherman’s Syndrome Treatment Centre in Jaipur for an accurate diagnosis and personalized care.
Cocoon Hospital offers a minimally invasive surgical procedure, such as hysteroscopic surgery (adhesiolysis), where no abdominal incisions are needed to visualize and remove uterine adhesions under direct view.
Our experienced gynecologists and obstetricians focus on comprehensive care, as intrauterine adhesions don't always need treatment; however, if required, the treatment is based on your severity, extent of intrauterine adhesions, patient fertility goals, and risk of recurrence.
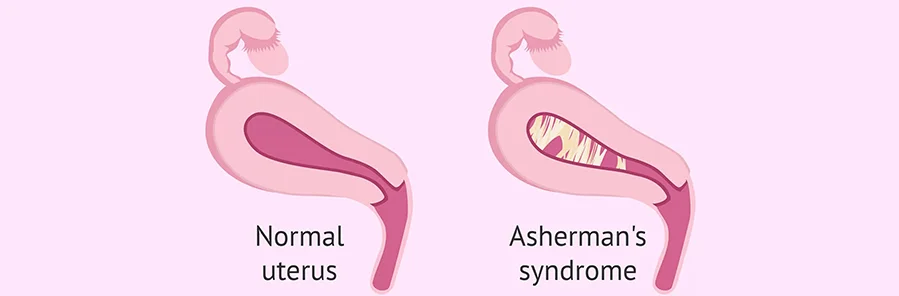
What is Asherman’s Syndrome
It is a condition where scar tissue (Adhesions) forms inside the womb or cervix, often fusing uterine walls and distorting the cavity.
Here are its key aspects:
| Main Aspect | Key Details |
|---|---|
| Cause | Mainly results from trauma to the uterine lining such as dilation and curettage (D&C) after miscarriage, abortion, or delivery. Other factors may include infections (e.g., tuberculosis), endometrial surgery, or radiation. |
| Characteristics | Formation of intrauterine adhesions or scar tissue that partially or fully fuse the uterine walls, leading to distortion of the uterine cavity. |
| Severity Level | Classified as mild (<1>moderate (1/3–2/3 affected), or severe (>2/3 of the cavity fused). |
| Symptoms Feel Like | Absence of periods (amenorrhea), very light periods (hypomenorrhea), infertility, recurrent miscarriages, and pelvic pain. Mild cases may show no symptoms. |
| Treatment Required? | Not always required. Mild or asymptomatic cases may be monitored, while moderate or severe cases with symptoms (especially infertility) often require hysteroscopic adhesiolysis. |
| Seriousness | Can be serious in moderate or severe forms due to infertility, pregnancy loss, and pain. It is not life-threatening but may significantly affect quality of life and fertility goals. Often treatable with hysteroscopic adhesiolysis surgery. |
| Fertility Impact | Yes. It may reduce fertility by distorting the uterine cavity, impairing embryo implantation, and increasing the risk of miscarriage. |
Signs That Indicate the Need for Asherman’s Syndrome Treatment
Not every scar tissue (adhesions) that forms inside the womb requires treatment. Mild or asymptomatic cases can be monitored
However, gynecologists and obstetricians in Jaipur usually recommend surgery when any of these signs interfere with daily activities, fertility, work, sleep, or emotional well‑being.
Your gynecologist will discuss medical or procedural treatment options based on your symptoms and personal preference.
| Symptoms Signalling Treatment | What Happens | Treatment Required |
|---|---|---|
| Infertility or Recurrent Miscarriages | Adhesions prevent proper embryo implantation, indicating the need for adhesiolysis to restore uterine cavity space. | High – Intervention may help restore fertility potential. |
| Amenorrhea (No Periods) | Complete fusion of the uterine cavity blocks menstrual flow, requiring intervention to restore normal uterine function. | Critical – Surgery is often necessary to reopen the uterus. |
| Hypomenorrhea (Very Light Periods) or Cyclic Pelvic Pain | Suggests partial obstruction or trapped menstrual blood, commonly seen in moderate cases. | Moderate – Monitoring or adhesiolysis may be required depending on severity. |
Asherman’s Syndrome Diagnosis
At Cocoon Hospital, diagnosis is usually through imaging and direct visualization to confirm intrauterine adhesions, often suspected from symptoms such as infertility or absent periods.
- Diagnostic hysteroscopy: The go-to test for diagnosing Asherman’s syndrome.
- Hysterosalpingography (HSG) with dye and X-rays or saline sonohysterography (SIS) detects cavity irregularities.
- MRI: Used in complex cases.
- 3D Ultrasound: Sometimes used to visualize the uterine cavity structure.
Uterine Asherman’s Syndrome Options in Jaipur
How is it Treated?
It doesn't always require treatment, particularly for mild or asymptomatic cases. The treatment decisions hinge on your symptoms, pregnancy history, and future plans for pregnancy.
Is Surgery Always Required?
No. Hysteroscopic adhesiolysis is the definitive surgical treatment for symptomatic moderate-to-severe cases.
Key Aspects of Hysteroscopic Adhesiolysis
Here are the key details that you should know:
| Key Aspects | Description |
|---|---|
| What It Is | A minimally invasive procedure using a thin, lighted hysteroscope inserted through the cervix to visualize and remove uterine adhesions. It restores the normal uterine cavity shape without abdominal (belly) cuts. |
| Ideal Candidate | Women with confirmed intrauterine adhesions causing infertility, amenorrhea, hypomenorrhea, or recurrent miscarriage. Often associated with a history of dilation and curettage (D&C), infection, or postpartum curettage. |
| Who Is Not an Ideal Candidate | Not suitable for women with active infection, pregnancy, or uterine malignancy. |
| Procedure Steps | Preparation: Anesthesia, lithotomy position (lying on the back with legs in stirrups), and imaging consent. Insertion: A thin hysteroscope is inserted through the vagina and cervix; saline fluid is used to expand the uterine cavity. Adhesiolysis: Adhesions are cut using scissors, forceps, or blunt dissection under ultrasound guidance. Completion: Placement of an IUD/balloon and hyaluronic gel to prevent recurrence. Duration: Typically 15–60 minutes; usually performed as a same-day procedure. |
| Safety Profile | Considered a safe, effective, minimally invasive treatment for intrauterine adhesions (IUA). Recurrence risk is low when postoperative estrogen therapy and barrier methods are used. |
| Complications | Possible risks include uterine perforation, bleeding, infection, fluid overload, and cervical trauma. These risks are minimized with proper technique and ultrasound guidance. |
Recovery After Hysteroscopic Adhesiolysis
The recovery may vary based on the type, severity of the condition, and other individual factors. Most individuals return to normal, light activities within 1–2 days, and full recovery takes about 4–6 weeks.
Here are some of the key tips:
- Take prescribed hormones (estrogen) and antibiotics to avoid re-adhesion.
- Watch for fever, heavy bleeding, and foul discharge; if you notice these, call your doctor.
- Fertility: Wait 3 months before trying IVF or pregnancy.
Asherman’s Syndrome Treatment Cost in Jaipur
The Asherman’s Syndrome treatment cost in Jaipur depends on the following:
- Procedure complexity
- Room category and hospital stay
- Patient’s medical condition
- Number of sessions
- Post-operative hormonal therapy
Approximate cost range: ₹25,000 to above ₹70,000 per session.
Why Choose Cocoon Hospital for Intrauterine Adhesions Treatment in Jaipur?
Cocoon Hospital is the leading Asherman’s Syndrome treatment center in Jaipur, combining minimally invasive hysteroscopic adhesiolysis with cutting-edge technology backed by compassionate care tailored to every woman.
Our multidisciplinary team combines clinical expertise with a patient-centred approach for the best pregnancy-related outcome and recovery.
Heres what makes Cocoon stand out:
- Women-Centric Focus
- Experienced Surgical Team
- Modern Diagnostic Tools and Laparoscopic Equipment
- Post-Operative Support and Follow-Up Care
- We Have Performed Over 10,000+ Gynecological Surgeries
Ready to Get the Right Intrauterine Adhesions Treatment in Jaipur
Speak to our team for expert guidance at 08929816349.
Our Address: Airport Plaza, Tonk Rd, Chandrakala Colony, Mata Colony, Jaipur, Rajasthan
FAQs
Is Asherman’s Syndrome curable ?
Yes, however, the success depends on severity and timely treatment.
Can Asherman’s Syndrome cause Infertility?
Yes. It can disrupt the uterine lining and cavity, increasing the risk of infertility or miscarriage.
Is Hysteroscopic Surgery safe ?
Yes. It is a safe and minimally invasive procedure when performed by experienced doctors.
Can periods return after Asherman’s Syndrome treatment?
In many cases, normal or improved menstrual flow returns after surgery. The success depends on the severity and timely treatment.
Can Asherman’s Syndrome recur?
Recurrence is possible because of extensive initial adhesions, dense scar tissue, or underlying issues such as endometrial tuberculosis. But proper post-operative care significantly lowers the risk.
Medically Reviewed & Updated
Reviewed by Dr. Anupama Gangwal, Senior Consultant Obstetrics & Gynecology, on 04 May 2026.
Meet Our Doctors
Know more
Latest from blogs
Learn more
Conditions
- Abnormal Uterine Bleeding
- Uterine Fibroids
- Uterine Prolapse Treatment
- Adenomyosis Treatment
- Uterine Septum Treatment
- Uterine Polyps Treatment
- Asherman’s Syndrome Treatment
- Ovarian Cyst Treatment
- Adnexal Masses Treatment
- What is Pelvic Inflammatory Disease
- Pelvic Pain Treatment
- Retained IUCD Treatment
- Hydrosalpinx Treatment
- Ectopic Pregnancy Treatment
- Tubal Block Treatment
- Urinary Problems Treatment
- Cervical Cancer Treatment
- Congenital Malformation of Uterus Treatment
- Endometrial Cancer Treatment
- Ovarian Cancer Treatment
Quick Enquiry
Fill the form below and we will get back to you asap.

